An in vitro Reconstructed Normal Human Corneal Tissue Model for Corneal Drug Delivery Studies of Ophthalmic Formulations
- TR Number: 803
- Authors: Yulia Kaluzhny, Miriam Kinuthia, Viktor Karetsky, Laurence d’Argembeau-Thornton, Patrick Hayden and Mitchell Klausner
- Keywords: EpiCorneal, COR-100, drug delivery, ophthalmic drug delivery, ophthalmic drug development, drug transporters, ALDH-A1, TXNRD1,MUC4, ABCC1 efflux transporter, ABCB1 efflus transporter. Aldehyde dehydrogenase (ALDH-3A1), TEER
- Materials Tested: Sodium fluorescein, Lucifer yellow, rhodamine B, ofloxacin, voriconazole, benzalkonium chloride, EDTA, fluorescein isothiocyanate-labeled dextran (FD-4), cetyl pyridinium chloride, polyoxyethelene-20 stearyl ether
Purpose: Permeation of topically applied ocular drugs occurs predominantly through the cornea and therefore absorption studies using corneal tissues play a critical role in ocular drug formulation. Currently, most ocular absorption studies use in vivo or ex vivo animal tissues that have many disadvantages including poor standardization, species extrapolation, high cost, and ethical concerns.
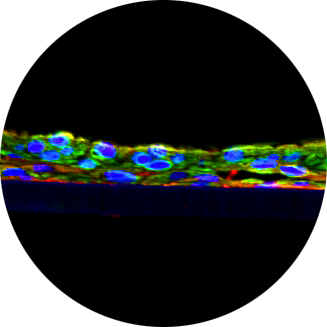
Methods: A reconstructed corneal tissue model (EpiCorneal™) was recently developed. The model consists of normal human corneal epithelial cells that have been cultured using serum-free medium to form a highly differentiated organotypic corneal epithelial tissue. The multilayered cultures contain tight junctions and develop barrier properties comparable to the in vivo human cornea. Real-time qPCR confirmed that the reconstructed tissues express ALDH-A1 and TXNRD1 (corneal epithelium-specific enzymes that confer resistance to UV light damage), MUC4 (corneal glycoprotein mucin), and ABCC1 and ABCB1 (efflux transporters with important roles in corneal drug distribution). The permeability of the model was evaluated using compounds with a wide range of properties: a) the hydrophilic dyes sodium fluorescein (NaFl), fluorescein isothiocyanate-labeled dextran (FD-4, MW=4000), and lucifer yellow (LY); b) the hydrophobic dye rhodamine B (RdB), and c) ophthalmic related antibiotics, ofloxacin (OFL) and voriconazole (VCZ). The effect of permeation enhancing agents, 0.01% Benzalkonium Chloride (BAK), 0.05-0.5% EDTA, 0.005% Cetylpyridinium chloride (CPC), and 0.02% Polyoxyethelen-20 stearyl ether (PSE), was investigated.
Results: The permeation coefficient (Kp) for NaFl/ FD-4/ LY/ RdB/ OFL/ and VCZ was 6.0±0.1×10-7/ 5.7±3.8×10-8/ 6.8±0.7×10-7/ 3.5±0.4×10-5/ 1.0±0.2×10-6/ and 3.9±1.1×10-5 cm/s. The Kp’s agree with literature values. 0.25% EDTA increased permeability of NaFl/ FD-4/ LY/ and VCZ by 2.2/ 3.9/ 7.1/ and 4.0 fold, respectively. 0.01% BAC increased the permeability of OFL and VCZ by 3.4 and 18.5 fold, respectively. 0.02% PSE increased the permeability of NaFl and FD-4 by 4.1 and 3.0 fold, respectively.
Conclusion: The reconstructed in vitro EpiCorneal tissue morphology, barrier properties, and permeability resemble those of the in vivo human cornea. This model is anticipated to be a useful tool to evaluate new corneal drug formulations.
Note: Subsequent to submission of this abstract, additional data on corneal wound healing were obtained which have been included in this presentation.