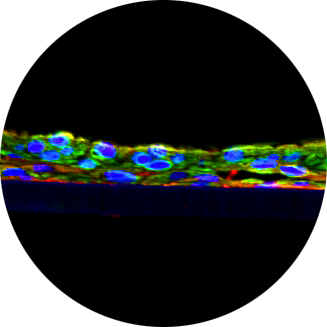
TISSUE ENGINEERED IN VITRO HUMAN AIRWAY MODELS (EPIAIRWAY) OF ASTHMA AND COPD.
- TR Number: 521
- Authors: Hayden, P.J., Jackson, Jr., G.R., Bolmarcich, J., and Klausner, M. MatTek Corporation, Ashland, MA.
- Keywords: Airway epithelial cells, Airway smooth muscle cells, Asthma, COPD, Chronic Obstructive Pulmonary Disease (COPD), Cytokeratin-17, Emphysema, Eotaxin-1, Eotaxin-3, EpiAirway, EpiAirway-FT, EpiAirwayFT, Goblet cell hyperplasia, Goblet cells, Human pulmonary fibroblasts, IL-8, INFa/b, IP-10, MIP-3a, Muscle cells, Nonsmoker, Poly(I:C), RANTES, Respiratory disease, Smoker, Smooth muscle actin, TARC, TH2 cytocines, TSLP, Tight junctions, Viral challenge
- Materials Tested: IL-13, IL-4, TNF-a
This study by scientists at MatTek Corp. demonstrated that MatTek’s EpiAirway and EpiAirway-FT in vitro human tracheal/bronchial tissue equivalents can be produced from airway epithelium of diseased individuals, and that these tissues are excellent in vitro human models of asthma and COPD providing important unique attributes that animal models cannot provide, including the ability to address human individual variability and genetic factors, and a means to determine mechanisms of human virus elicitation of asthma and COPD exacerbations. INTRODUCTION: Asthma and chronic obstructive pulmonary disease (COPD) are the two leading chronic respiratory diseases in the US. However, reliable in vitro human models are not widely available to researchers attempting to understand asthma and COPD pathogenesis and develop therapeutic interventions for these diseases. Here we report on a program to create and maintain a human cell bank derived from airway epithelium of diseased individuals, and production of tissue engineered in vitro human models of asthma and COPD from the cells. METHODS: Tracheal and bronchial tissues are obtained from non-transplantable organs donated from normal, asthmatic or COPD individuals with IRB approval and informed consent. Epithelial and mesenchymal cells are isolated from the tissues, cryopreserved and maintained in a cell bank. As needed, cell are recovered and utilized to produce in vitro tissue engineered models. RESULTS: Sixteen lung samples have been processed to-date. The airway histopathology of each donor was evaluated. Airway epithelial cells, fibroblasts and smooth muscle cells isolated from the lung tissues (7 normal, 6 asthma and 3 emphysema donors). Cells were characterized morphologically and by immunocytochemistry. Tissue engineered models were cultured at the air-liquid interface and consist of well-differentiated human tracheal/bronchial epithelium (EpiAirway™) as well as human airway epithelium co-cultured with donor-matched human airway mesenchymal cells (EpiAirway-FT™). H&E stained paraffin sections show development of pseudostratified epithelium with mucociliary phenotype similar to in vivo proximal airway epithelium. Transmission electron microscopy shows development of tight junctions and transepithelial electrical resistance measurements demonstrate barrier function. The cultures exhibited in-vivo like responses including stimulation of mucus production by TH2 cytokines and secretion of various cytokines and chemokines after stimulation with innate immune challenges and TH1/TH2 cytokines. CONCLUSIONS: These in vitro human models of asthma and COPD provide important unique attributes that animal models cannot provide, including the ability to address human individual variability and genetic factors and a means to determine mechanisms of human virus elicitation of asthma and COPD exacerbations. These models will provide researchers important new tools for investigating the role of airway epithelium and mesenchymal cells in asthma and COPD pathogenesis and development and testing of new therapeutic treatments for these diseases.