The Impact of Over-The-Counter Lactic Acid Containing Vaginal Gels on the Integrity and Inflammatory State of the Vaginal Epithelium in vitro
- TR Number: 992
- Authors: David Tyssen, Anna C. Hearps, Kalyani Guntur, Lindi Masson, Simon Cook, Simon E. Moulton, Jacques Ravel, Catriona S. Bradshaw, Seyoum Ayehunie and Gilda Tachedjian
- Keywords: EpiVaginal (VEC-100), lactic acid, lactobacilli, vaginal gel, vaginal microbiome, Caya Diaphragm Gel, ContraGel green, Lactigel, Relactagel, Geliofil Classic, Balance Activ, Canesbalance, Gynofit, Restore, Aci-Jel Balance, Fleurstat (1% astodrimer), Gynol II, hydroxyethyl cellulose, Lubricant, Diaphragm gel, Vaginal moisturizer, pH balance, IL-1b, IL-6, IL-1a, IL-1RA, IL-8, MIP-3a, TEER, barrier integrity, hyperosmolal gels, loss of glycogen layers, epithelial thinning, epithelial layer separation, epithelial reorganization, tissue damage, bacterial vaginosis, inflammation, vaginal irritation, osmolality, vaginal microbiome
- Materials Tested: Caya Diaphragm Gel, ContraGel green, Lactigel, Relactagel, Geliofil Classic, Balance Activ, Canesbalance, Gynofit, Restore, Aci-Jel Balance, Fleurstat, Gynol II, hydroxyethyl cellulose
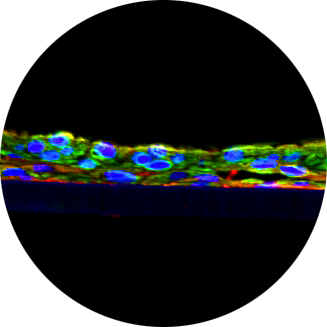
The vaginal microbiome influences a wide range of health outcomes in women, where a microbiome dominated by Lactobacillus spp. is considered optimal and associated with reduced risk of pre-term birth and acquisition of sexually transmitted infections including HIV. Conversely, replacement of lactobacilli by non-optimal bacteria leads to the development of bacterial vaginosis, which is associated with increased risk of these outcomes. Lactobacilli produce the metabolite lactic acid (LA) which is a potent antibacterial and antiviral agent. The potential therapeutic benefits of LA have prompted the development of numerous over-the-counter LA-containing gels for use in the vagina, although a comprehensive analysis of the impact of these formulations on the cervicovaginal epithelium and pro-inflammatory cytokine/chemokine responses, has not been assessed. Here, we evaluated the properties of 11 over-the-counter gels, including 9 containing LA, marketed for use in the vagina. Ten of the 11 gels had an osmolality greater than vaginal fluid from women with Lactobacillus-dominated microbiota (370 ± 40 mOsmol/kg in women with Nugent score 0–3), with six gels that were hyperosmolal >2,000 mOsmol/kg. Using a reconstructed primary cell model of the vaginal epithelium, we found hyperosmolal gels had a detrimental impact on epithelial barrier integrity, resulting in substantial cellular toxicity (<10% viability as compared to untreated cells) and reduced epithelial barrier integrity [≈30%of untreated cells, assessed by transepithelial electrical resistance (TEER)]. Treatment of vaginal tissues with most of the gels elicited the production of pro-inflammatory factors including IL-1a (8 of 11) and IL-1b (10 of 11) which are associated with heightened risk of HIV acquisition in vivo. The majority of the OTC gels elicited moderate tissue damage as determined by histology. The detrimental effects of these gels on the human vaginal epithelium in vitro may predict compromised epithelial barrier integrity and genital inflammation in vivo, which has implications for sexual and reproductive health. This study highlights the importance of evaluating the impact of intravaginal products on the integrity and inflammatory status of the mucosal epithelium to avoid unfavorable off target effects.