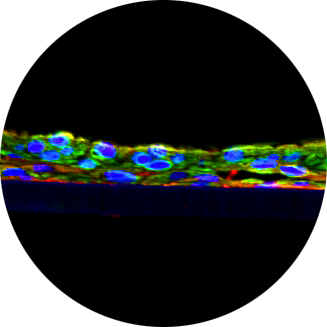
TH2 CYTOKINE STIMULATED AIRWAY EPITHELIAL CELLS DEMONSTRATE GRANULE-DEPENDENT FasL LOCALIZATION.
- TR Number: 410
- Authors: Singhera, G.K., Sekhon, M.S., Dorscheid, D.R. The James Hogg iCAPTURE Centre for Cardiovascular and Pulmonary Research, St. Paul’s Hospital / Providence Health Care-University of British Columbia, Vancouver, BC, Canada.
- Keywords: Airway epithelial, Antibodies, Asthma, Bronchiolar lumen, CD63, Crm-1, Cytokine stimulation, EpiAirway, Fas ligand, FasL, GM-CSF, IL-3, IL-5, Immune barrier, Inflammation, Inflammatory, Inflammatory challenge, P62, Protein expression, TH2
- Materials Tested: Granulocyte macrophage colony stimulating factor (GMCSF), IL-3, IL-5
This study by researchers at St. Paul’s Hospital / University of British Columbia demonstrated how MatTek’s EpiAirway human airway tissue equivalent can be used to investigate if the localization and presentation of an airway epithelial cell constituent, Fas Ligand (FasL), is dependant on the inflammatory state of the airway tissue. Background: Airway epithelium has been the target of asthma research and it has been suggested that it serves as an immune barrier. Rationale: Constitutive or inducible expression of Fas Ligand (FasL) has been demonstrated in epithelial cells. Little is known about the regulation and localization of FasL. Expression of FasL has been associated with the establishment of immune privilege against immune cells. However, if FasL presentation is dysregulated it may lead to inappropriate inflammation as seen in asthma. Hypothesis: FasL localization and presentation in airway epithelial cells is dependant upon the inflammatory environment. Methods: Researchers at St. Paul’s Hospital / University of British Columbia (Canada) treated normal airway epithelial cells with IL-3, IL-5 and GM-CSF for 1h, and treated EpiAirway differentiated human airway epithelium with IL-3, IL-5 and GM-CSF for 1h and 4h. Confocal microscopy, flow cytometry, immunoprecipitation and Western blot analysis were conducted to analyze cell-surface protein expression, cellular localization and total protein expression of FasL and the potential co-localizing molecules CD63, p62 and exportin-1. Results: Using confocal microscopy FasL was localized in a perinuclear distribution at rest and activation of these cells resulted in FasL translocation to the cell membrane. CD63 a marker of azurophilic granules, was found to be associated with this translocation. In the activated state CD63 and exportin-1 were increased on the cell surface relative to cells at rest. There was no change in p62. The TH2 inflammatory challenge resulted in an increase in FasL association with exportin-1 and p62 as detected by Immunoprecipitation. Conclusion: Our results suggest that TH2 inflammatory challenges may increase the epithelial immune barrier by increasing the presentation of FasL on the cell surface. This process involves exportin-1 and piecemeal degranulation. The inflammatory conditions the airway is exposed to may determine the state of the FasL-mediated immune barrier. Dysregulation of this translocation may contribute to conditions such as asthma.