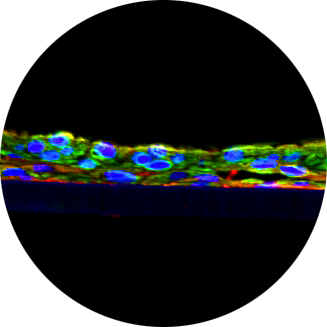
Shigella depends on SepA to destabilize the intestinal epithelial integrity via cofilin activation
- TR Number: 818
- Authors: Ana Maldonado-Contreras, James R. Birtley, Erik Boll, Yun Zhao, Karen L. Mumy, Juan Toscano, Seyoum Ayehunie, Hans-Christian Reinecker, Lawrence J. Stern, and Beth A. McCormick
- Keywords: Enteric pathogens, intestinal epithelial barrier, host-bacteria interactions, bacterial transit, tight junctions, SMI-100, F-actin organization, cofilin, phalloidin, epithelial desquamation, bacteria, cofilin; LIM Kinases; SepA; Shigella; SPATEs
- Materials Tested: dexamethasone, simvastatin, aphidicolin
Shigella is unique among enteric pathogens, as it invades colonic epithelia through the basolateral pole. Therefore, it has evolved the ability to breach the intestinal epithelial barrier to deploy an arsenal of effector proteins, which permits bacterial invasion and leads to a severe inflammatory response. However, the mechanisms used by Shigella to regulate epithelial barrier permeability remain unknown. To address this question, we used both an intestinal polarized model and a human ex-vivo model to further characterize the early events of host-bacteria interactions. Our results showed that secreted Serine Protease A (SepA), which belongs to the serine protease autotransporter of Enterobacteriaceae family, is responsible for critically disrupting the intestinal epithelial barrier. Such disruption facilitates bacterial transit to the basolateral pole of the epithelium, ultimately fostering the hallmarks of the disease pathology. SepA was found to cause a decrease in active LIM Kinase 1 (LIMK1) levels, a negative inhibitor of actin-remodeling proteins, namely cofilin. Correspondingly, we observed increased activation of cofilin, a major actinpolymerization factor known to control opening of tight junctions at the epithelial barrier. Furthermore, we resolved the crystal structure of SepA to elucidate its role on actin-dynamics and barrier disruption. The serine protease activity of SepA was found to be required for the regulatory effects on LIMK1 and cofilin, resulting in the disruption of the epithelial barrier during infection.
Altogether, we demonstrate that SepA is indispensable for barrier disruption, ultimately facilitating Shigella transit to the basolateral pole where it effectively invades the epithelium.