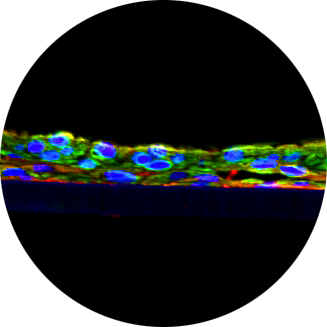
RECONSTRUCTION OF VAGINAL TISSUE MODEL FOR HIV INFECTION.
- TR Number: 246
- Authors: Ayehunie1, S., Cannon1, C.L., Kubilus1, J., Pudney2, J., LaBonte3, J., Anderson2, D., Sodroski3, J., and Klausner1, M. 1MatTek Corp., Ashland, MA 01721. 2Brigham and Womens Hospital, 3Dana Farber Cancer Institute, Boston, MA.
- Keywords: AIDS, Birbeck granules, CD19, CD1a, CD3, CD34, DC, Dendritic cells, Ectocervix, EpiVaginal, Gene expression, HIV, HLA-DR, Langerhans cells, Microbicide, Microbicides, Mucosal, NHVE, RNA expression, STD, T cell, Transcytosis, Vaginal tissue, Virus
The HIV/AIDS epidemic is continuing to escalate worldwide and it is estimated that through the year 2000, more than 34 million people have already been infected with the virus. Daily, 16,000 individuals acquire HIV-1 infection and the majority of all adult HIV infections (90%) are obtained through sexual contact. The cervico-vaginal tissues are thought to be important sites for heterosexual transmission of HIV to women. The proposed mechanisms of virus transmission across the mucosa include; 1) direct infection of epithelial cells, 2) transcytosis, 3) trauma that results in breaches in epithelial integrity, and 4) uptake by resident Langerhans cells. Understanding of viral and host factors of sexual transmission of HIV is essential to study HIV pathogenesis, protective vaccines, and therapeutic strategies. One of the main problems surrounding these issues is the lack of appropriate in vitro viral transmission models that mimic the in vivo stratified squamous epithelial layers present in the vagina and ectocervix of the female genital organ. Most of the currently available models for the study of HIV transmission utilize monolayers of primary epithelial cells, antigen presenting cells, T cells, or their cell line derivatives. These monolayer cultures lack the specialized multilayer vaginal tissue structure which may serve as a barrier or a trap for HIV infection. To circumvent the problems of monolayer cultures and to describe the in vivo phenomenon of HIV infection, researchers have been using either explants of vaginal/cervical tissues in an in vitro organ culture models or animal models such as the rhesus monkey. However, obtaining explants for routine use is difficult. Also, animal experiments are expensive, and utilize the related SIV (semian immunodeficiency virus) instead of HIV. Here scientists at Brigham and Women’s Hospital (Boston), Dana Farber Cancer Institute (Boston) and MatTek Corp. describe the development of EpiVaginal™, an in vitro vaginal tissue model that can serve as a valuable tool for immediate applicability to the development of vaginal microbicides. The EpiVaginal model is superior to current monolayer systems in that it provides the vaginal tissue architecture including the basal, parabasal, glycogenated intermediate, and the superficial surface layers. Additional advantages include; the cells are human derived, and requires less time to obtain results (when compared with monkey experiments), and is likely cost effective. Work is in progress to incorporate Langerhans cells/dendritic cells into the model.