Tissue Models
Organotypic 3D primary human nasal tissue model for toxicological studies
- TR Number: 963
- Authors: Seyoum Ayehunie, Michelle Debatis, Zachary Stevens, Julia Oh, Yulia Kaluzhny, Alex Armento
- Keywords: NAS-100, TEER, MTT viability CK19, tight junctions, ZO-1, Claudin-1, mucin MUC5B, MUC5AC, SARS-CoV-2 entry-related proteins, ACE-2, TMPRSS2, cilia, alpha-tubulin single cell sequencing, goblet cells, club cells, basal cells, multiciliated cells, not previously identified cells NPIC, allergic rhinitis, respiratory syncytial virus infection, IL1RL1, MMP9, MMP10, laminins, integrins, viral Infection, IDO1
- Materials Tested: rhinovirus, respiratory syncytial virus
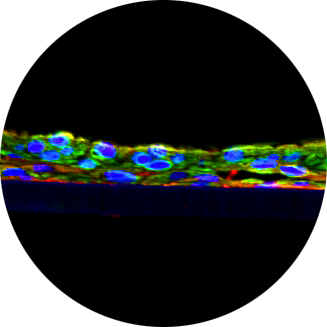
The nasal mucosa serves as the first line of defense against inhaled chemicals, drugs, and respiratory infections. Here we developed a novel in vitro primary human cell-based 3D human nasal epithelial tissue (NET) cultured on a cell culture insert with a porous (0.4 μm) membrane bottom at an air-liquid interface (ALI). The NET model was characterized by histology, barrier function (TEER), viability (MTT), toxicity, and infection with viruses. Histological and immunohistochemical evaluation of the in vitro NET showed a polarized, multilayered tissue that expresses markers of epithelial cells (CK19), tight junctions (ZO-1 and Claudin-1), mucin (MUC5B and MUC5AC), SARS-CoV-2 entry-related /proteins/genes (ACE-2 and TMPRSS2), and cilia (alpha-tubulin). Single cell sequencing of the differentiated NET also confirmed the presence of differentiated cell types (goblet, club cells, basal, multiciliated cells, and not previously identified cells (NPIC). The NPIC were enriched in response to allergic rhinitis/respiratory syncytial virus infection (increase in IL1RL1, MMP9, MMP10) and some laminins and integrins. Infection of the NET with viruses also showed high expression of IDO1, which is associated with innate antiviral immune functions. To monitor reproducibility, the MTT and TEER results from N=9 lots were analyzed: MTT OD values were >1.0 (mean OD =1.7±0.2) and TEER values were 300.9±42.4 Ω*cm2 (n=9 lots). To evaluate the utility of the nasal tissue model for toxicological studies, we tested the effect of a known mucous membrane irritant, butylamine, following 4 hr topical exposure to 0.5 mg/mL and 2 mg/mL of the test article. The irritant reduced the barrier integrity to 33.2% ± 0.0 and 12.3% ± 5.8, respectively, compared to the vehicle control (corn oil), which is indicative of toxicity of the test article. In short, this novel NET model can be added to the toxicologist’s toolbox of 3D respiratory tissue models to predict safety of chemical inhalants, therapeutic candidates, viral and bacterial infections at the inhalation entry site.