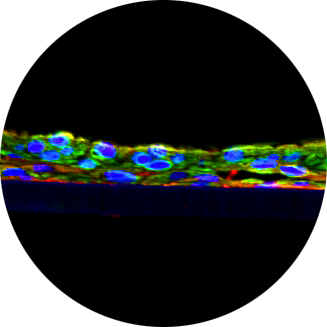
NOVEL 3D HUMAN SMALL INTESTINAL TISSUE MODEL (EPIINESTINAL™ ) TO ASSESS DRUG PERMEATION & INFLAMMATION
- TR Number: 763
- Authors: Seyoum Ayehunie1, Zachary Stevens1, Timothy Landry1, Mohammed Taimi2, Mitchell Klausner1, and Patrick Hayden1. 1MatTek Corporation, Ashland, MA 01721 and 2Apredica, 313 Pleasant Street, Watertown, MA.
- Keywords: EpiIntestinal (SMI-100-FT, SMI-100), Drug transport, Drug permeation,Caco-2, Efflux drug transporters,P-glycoprotein, MDR1,MRP1, MRP2, Breast cancer resistance protein (BCRP), Brush borders, Tight junctions, Mucous secretory granules, TEER, IL-6, IL-8, GRO-a, Long term culture, Lot-to-lot reproducibility, Cytokeratin 19, Cell migration
- Materials Tested: Ranitidine, Talinolol, Warfarin, Verapamil, TNF-a, IFN-g, Lucifer yellow
Purpose: Drug transport and permeability across the small intestine (SMI) is a key parameter for determining bioavailability of orally administered drugs. The currently available in vitro models are highly dependent on immortalized cell lines (e.g. Caco-2) and have significant deficiencies for drug development applications. Therefore, we developed an in vitro SMI model (EpiIntestinalTM) using normal human intestinal cells which closely recapitulates the physiology, 3D tissue architecture, and function of the small intestine for use in pharmaceutical development applications and inflammation. Methods: Normal human primary SMI epithelial cells, fibroblasts, and endothelial cells were harvested from primary tissue and expanded in monolayer culture and seeded onto microporous membrane inserts to reconstruct the 3D SMI tissues. The 3D tissues were characterized phenotypically, (H&E, immunohistochemistry, and TEM), physiologically (TEER), and for gene expression (RT-PCR). Functionally, drug permeation was analyzed using LC-MS/MS and inflammatory responses were measured by BioPlex ELISA. Results: Characterization of the in vitro SMI tissue model showed: 1) wall-to-wall tissue growth which makes it ideal for apical (lumen-like) application of drugs, 2) columnar epithelial cell morphology, 3) TEER in the physiological range of 60-180 Ώ*cm2 mimicking the SMI microenvironment in vivo, 4) formation of brush borders and tight junctions, 5) gene expression of the prominent efflux drug transporters such as P-glycoprotein (P-gp, MDR-1) and BCRP, and 6) extended life span (up to 30 days) in culture. Permeation studies of drugs (ranitidine and talinolol) showed efflux ratios >2 fold indicative of P-gp efflux transport. Exposure of the SMI tissue to proinflammatory cytokines (TNF-α and IFN-γ) induced upregulation of cytokines/chemokines such as IL-6, IL-8, and GRO-α. Conclusions: The newly developed SMI tissue model will have application in drug safety and inflammation studies. Availability of an easy-to-use, economical, and reproducible in vitro reconstructed human SMI tissue will reduce animal use, minimize the number of test compounds dropped due to permeation problems in Caco-2, and significantly improve the prediction potential for drug absorption or inflammation in humans for candidate pharmaceutical compounds.