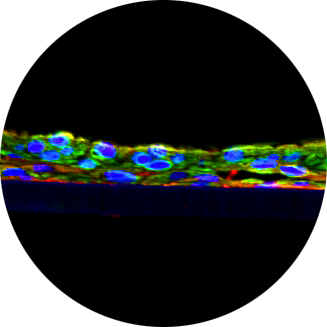
Molecular Mechanism of Ocular Surface Damage: Dry Eye and Wound Healing Models Using in vitro Reconstructed Human Corneal Tissues
- TR Number: 805
- Authors: Yulia Kaluzhny, Mitchell Klausner, Miriam Kinuthia, Alena Plotkin, and Patrick Hayden
- Keywords: Dry eye, corneal wound healing, EpiCorneal, COR-100, dessicating stress conditions, TEER, gene analysis, EGF receptor, punch biopsy, abrasion, desmosomes, ZO-1, microvilli, tight junctions, scratch wound, cytokeratin 3/12, eye drops, mucin-1, MUC1, IL-1a, IL-1b, transglutaminase-1
- Materials Tested: NaOH, Erlotinib, conditioned media, GenTeal eye drops, Contrived Tears eye drops
Current methods used to investigate mechanisms of corneal wound healing (CWH) and pathogenesis of dry eye disease (DED) utilize monolayer cell cultures or animals, but there is a need for more physiologically relevant, human-based in vitro models for ocular surface research.
This study utilized the EpiCorneal tissue model comprised of normal human corneal epithelial cells that are cultured at the air-liquid interface. Corneal wounds were introduced by abrasion or chemicals (1N NaOH). Wounded tissues were cultured in the presence or absence of human corneal keratocytes (HCK) or the EGFR inhibitor (erlotinib, 10 uM). A DED model was generated by placing EpiCorneal tissues under desiccating stress conditions (DSC, 40% RH, 40°C, and 5% CO2) that induce morphological, cellular, and molecular changes relevant to dry eye.
CWH was analyzed by transepithelial electrical resistance (TEER), histology, confocal microscopy, and gene expression. TEER recovered to 934/502 Ω*cm2 in the presence/or absence of HCK after 4 days post-abrasion. mRNA expression was analyzed using a 96-gene wound healing microarray. 2 genes were significantly up-regulated in the EpiCorneal tissues 24h post-abrasion in the absence of HCK and 12 genes (from the WNT, FGF, small GTPases, chemokine, collagen, integrin, and protein kinase families) were up-regulated in the presence of HCK. DED was analyzed by TEER, histology, tissue viability, mucins, release of pro-inflammatory cytokines, and gene expression. Dramatic reduction in tissue thickness was observed after 48h in DSC that coincided with decreased expression of mucins, increased TEER and up-regulation of cross-linking genes (TGM1). Topical application (25 μl/tissue) of lubricant gel drops (GenTeal, Alcon) or artificial tears (Ursa Bioscience) improved tissue morphology and barrier function.
The results demonstrated that the in vitro organotypic human corneal tissue structurally and functionally reproduces CWH and DED. The model will avoid species extrapolation, be more cost effective and more reproducible than animal methods, and will facilitate drug discovery by allowing screening and optimization of active pharmaceuticals prior to clinical studies.