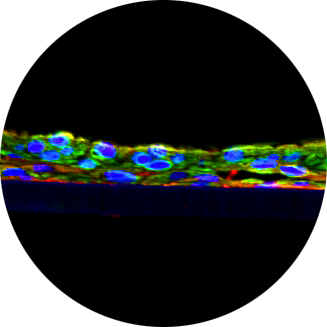
Modeling SARS-CoV-2 and Influenza Infections and Antiviral Treatments in Human Lung 2 Epithelial Tissue Equivalents
- TR Number: 932
- Authors: Hoda Zarkoob, Anna Allué-Guardia, Yu-Chi Chen, Olive Jung, Andreu Garcia-Vilanova, Min Jae Song, Jun-Gyu Park, Fatai Oladunni, Jesse Miller, Yen-Ting Tung, Ivan Kosik, David Schultz, Jonathan Yewdell, Jordi B. Torrelles, Luis Martinez-Sobrido, Sara Cherry, Marc Ferrer, Emily M. Lee
- Keywords: SARS-CoV-2 virus, COVID-19, infection, viral replication, EpiAirway (AIR-100), EpiAlveolar (ALV-100-FT-PE12), ACE2, TMPRSS2, NRP-1, α-tubulin, MUC5AC, KRT5, F-actin filaments, N-protein (NP), Phalloidin, alveolar type I, AQP5, alveolar type II, surfactant protein (SP-B), CD31, vimentin, aquaporin, surfactant-C, influenza A, H1N1 IAV strains A/Puerto Rico/8/1934 (PR8), pandemic A/California/07/2009 (pH1N1), SARS-CoV-2/WA/2020/D614, clinical isolate, cytokeratin 5, ciliated cells, goblet cells, secreted virus, Th1, Th2, Th17, IFN-alpha, IFN-beta, type II interferon, IFN-gamma, type III interferon, IFN-lambda, IL-28A, EN-RAGE/S100A12, neutrophil development, remdesivir, cyclosporine, hydroxychloroquine, camostat, TMPRSS2 inhibitor, nelfinavir, anti-retroviral, zanamivir, oseltamivir, salinomycin, Hoechst, goblet cells, cilliated cells, IL-18, TNF-alpha, TNF-beta, IL-1beta, hepatocyte growth factor (HGF), IL-7, interleukin 6 (IL-6), C-X-C motif chemokine ligand 10 or interferon gamma induced protein 10 (CXCL-10/IP-10), C-C motif ligand 3 or macrophage inflammatory protein 1alpha (CCL3/MIP-1alpha), C-C motif ligand 2 or monocyte chemoattractant protein-1 (CCL2/MCP-1), interleukin-1 receptor antagonist 1a (IL-1RA), granulocyte colony-stimulating factor (G-CSF), IL-1beta
- Materials Tested: cyclosporine, hydroxychloroquine, camostat, nelfinavir, anti-retroviral, zanamivir, oseltamivir, salinomycin, influenza A, H1N1 IAV strains A/Puerto Rico/8/1934 (PR8), pandemic A/California/07/2009 (pH1N1), SARS-CoV-2/WA/2020/D614, COVID-19
Sever acute respiratory syndrome coronavirus-2 (SARS-CoV-2) is the third coronavirus in less than 20 years to spillover from an animal reservoir and cause severe disease in humans. High impact respiratory viruses such a pathogenic beta-coronaviruses and influenza viruses, as well as other emerging respiratory viruses, pose an ongoing global health threat to humans. There is a critical need for physiologically relevant, robust and ready to use, in vitro cellular assay platforms to rapidly model the infectivity of emerging respiratory viruses and discover and develop new antiviral treatments. Here, we validate in vitro human alveolar and tracheobronchial tissue equivalents and assess their usefulness as in vitro assay platforms in the context of live SARS-CoV-2 and influenza A virus infections. We establish the cellular complexity of two distinct tracheobronchial and alveolar epithelial air liquid interface (ALI) tissue models, describe SARS-CoV-2 and influenza virus infectivity rates and patterns in these ALI tissues, the viral-induced cytokine production as it relates to tissue-specific disease, and demonstrate the pharmacologically validity of these lung epithelium models as antiviral drug screening assay platforms.