INJURY ENHANCES TLR2 FUNCTION AND ANTIMICROBIAL PEPTIDE EXPRESSION THROUGH A VITAMIN D–DEPENDENT MECHANISM.
- TR Number: 437
- Authors: Schauber1, J., Dorschner1, R.A., Coda1, A.B., Büchau1, A.S., Liu2, P.T., Kiken1, D., Helfrich3, J.R., Kang3, S., Elalieh4, H.Z., Steinmeyer5, A., Zügel6, U., Bikle4, D.D., Modlin2, R.L. and Gallo1, R.L. 1Division of Dermatology, University of California, San Diego, and VA San Diego Healthcare System, San Diego, California, USA; 2Division of Dermatology, Department of Medicine, David Geffen School of Medicine, University of California, Los Angeles, Los Angeles, California, USA; 3Department of Dermatology, University of Michigan, Ann Arbor, Michigan, USA; 4Department of Medicine, Endocrine Unit, Veterans Affairs Medical Center, University of California, San Francisco, San Francisco, California, USA; 5Medicinal Chemistry and 6Corporate Research Business Area Inflammation, Schering AG, Berlin, Germany.
- Keywords: 1,25(OH)2 vitamin D3, Anti-microbial, Anti-microbial peptide expression, Anti-microbial peptides, Antimicrobial, Antimicrobial peptide expression, Antimicrobial peptides, CD14, CYP27B1, Cathelicidin, EpiDerm, Epidermis, Innate immune response, Innate immunity, Keratinocytes, Microbial components, Microbial invasion, TGF-b1, TLR2, Vitamin D receptor, Vitamin D3, Infectious disease research
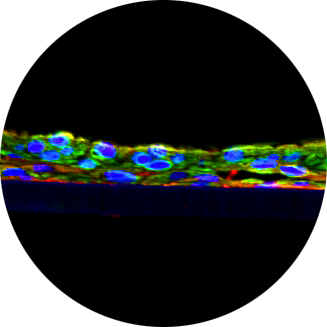
This study by researchers at UCSD, UCLA, UCSF, the University of Michigan and Schering AG demonstrated that MatTek’s EpiDerm human skin tissue equivalent can be used to study the effects of vitamin D3 on the human epidermis, specifically on keratinocytes, enabling them to recognize and respond to microbes, and to protect wounds against infection. An essential element of the innate immune response to injury is the capacity to recognize microbial invasion and stimulate production of antimicrobial peptides. In this study, researchers investigated how this process is controlled in the epidermis. Keratinocytes surrounding a wound increased expression of the genes coding for the microbial pattern recognition receptors CD14 and TLR2, complementing an increase in cathelicidin antimicrobial peptide expression. These genes were induced by 1,25(OH)2 vitamin D3 (1,25D3; its active form), suggesting a role for vitamin D3 in this process. How 1,25D3 could participate in the injury response was explained by findings that the levels of CYP27B1, which converts 25OH vitamin D3 (25D3) to active 1,25D3, were increased in wounds and induced in keratinocytes in response to TGF-â1. Blocking the vitamin D receptor, inhibiting CYP27B1, or limiting 25D3 availability prevented TGF-â1 from inducing cathelicidin, CD14, or TLR2 in human keratinocytes, while CYP27B1-deficient mice failed to increase CD14 expression following wounding. The functional consequence of these observations was confirmed by demonstrating that 1,25D3 enabled keratinocytes to recognize microbial components through TLR2 and respond by cathelicidin production. Thus, this research demonstrates what appears to be to be a previously unexpected role for vitamin D3 in innate immunity, enabling keratinocytes, including those found in EpiDerm human-keratinocyte-derived 3-D organotypic tissue constructs, to recognize and respond to microbes and to protect wounds against infection.