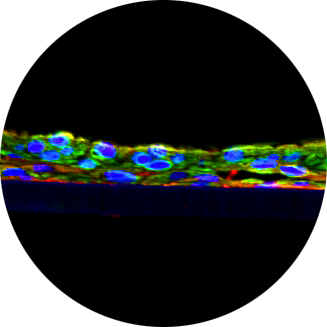
Induction of an Atopic Dermatitis-Like Phenotype in a Full-Thickness in vitro Human Skin Model
- TR Number: 849
- Authors: Patrick Hayden, Seyoum Ayehunie, Jonathan Oldach, and Mitchell Klausner
- Keywords: atopic dermatitis, EFT-400, Filaggrin, Involucrin, Ki67, Spongiosis, Cathelicidin, CCL27, CCL3, CCL5, Human beta defensin 1, hypogranulosis
- Materials Tested: clobetasol propionate
Atopic dermatitis (AD) is the most common inflammatory disease of the skin and is characterized by defects in keratinocyte differentiation and skin barrier dysfunction. The goal of the current work is to create an in vitro AD model for use in basic research and therapeutic development. To create the model, the in vitro full-thickness human skin model, EpiDermFT, was treated with a cocktail of Th2 cytokines to induce an AD phenotype. Following cytokine treatment, significant changes in differentiation markers, chemokines involved in T-cell recruitment, and skin barrier integrity were observed, closely resembling features found in AD skin in vivo. Specifically, differentiation markers such involucrin and filaggrin were down-regulated and the antimicrobial peptide, cathelicidin antimicrobial peptide (CAMP), and chemokines such as CCL3, CCL5, and, CCL27, were up-regulated at both the gene and protein level. Histological analysis revealed a thinner stratum corneum and spongiosis. Treatment with a corticosteroid, clobetasol propionate, was able to partially restore normal epidermal morphology and reverse expression of the AD biomarkers. These findings demonstrate that the model is consistent with the key hallmarks of AD and that it may be a useful tool for testing therapeutic formulations.