CYTOKINE AND CHEMOKINE RELEASE UPON PROLONGED MECHANICAL LOADING OF THE EPIDERMIS.
- TR Number: 462
- Authors: Bronneberg1, D., Spiekstra2, S.W., Cornelissen1, L.H., Oomens1, C.W.J., Gibbs2, S., Baaijens1, F.P.T. and Bouten1, C.V.C. 1Department of Biomedical Engineering, Eindhoven University of Technology, Eindhoven, The Netherlands. 2Department of Dermatology, VU University Medical Center, Amsterdam, The Netherlands.
- Keywords: CCL2/MCP-1, CCL20/MIP-3a, CXCL1/GRO-á, Cell damage, Cell membrane integrity , Cell swelling, Chemokines, Cytokines, EPI-100-MMHCF, EPI-200, EpiDerm, GRO-a, Interleukin 1 receptor antagonist (IL-1ra), Interleukin 1a (IL-1a), Interleukin 8, Lactate dehydrogenase (LDH), MCP-1, MIP-3a, Mechanical loading, Mechanically-induced skin damage, Necrosis, Pressure ulcer, TNF-a, Tumor necrosis factor alpha, Vacuoles
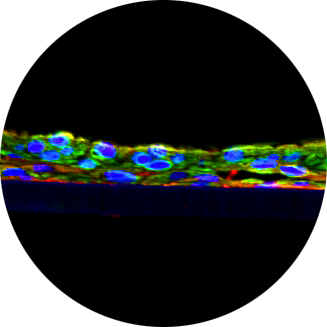
This study by researchers at the Eindhoven University of Technology and the VU University Medical Center Dept. of Dermatology demonstrated that MatTek’s EpiDerm human epidermal tissue equivalent can be used to study the damage caused by subjecting these epidermal tissues to increasing pressures for 24 hours, and that the resulting epidermal tissue damage could be assessed by histological examination (H&E staining) and by evaluation of the cell membrane integrity (lactate dehydrogenase (LDH) release). At this moment, pressure ulcer risk assessment is dominated by subjective measures and does not predict pressure ulcer development satisfactorily. Objective measures are, therefore, needed for an early detection of these ulcers. This in vitro study by researchers in the Eindhoven University of Technology Dept. of Biomedical Engineering and the VU University Medical Center Dept. of Dermatology evaluated cytokines and chemokines [interleukin lá (IL-lá), interleukin 1 receptor antagonist (IL-1RA), tumor necrosis factor á (TNF-á) and inter-leukin 8 (CXCL8/IL-8)] as early markers for mechanically-induced epidermal damage. Various degrees of epidermal damage were induced by subjecting commercially available epidermal equivalents (EpiDerm™) to increasing pressures (0, 50, 75, 100, 150, and 200 mmHg) for 24 h, using a loading device. At the end of the loading experiment, tissue damage was assessed by histological examination and by evaluation of the cell membrane integrity. Cytokines and chemokines were determined in the culture supernatant. Sustained epidermal loading resulted in an increased release of IL-lá, IL-lRA/TNF-á and CXCL8/IL-8. This was first observed at 75 mmHg, when the tissue was only slightly damaged. Swollen cells, vacuoles, necrosis and affected cell membranes were observed at pressures higher than 75 mmHg. Furthermore, at 150 and 200 mmHg, the cells in the lower part of the epidermis were severely compressed. In conclusion, IL-lá, IL-1RA, TNF-á and CXCL8/IL-8 are released in vitro as a result of sustained mechanical loading of the epidermis. The first increase in cytokines and chemokines was observed when the epidermal tissue (EpiDerm) was only slightly damaged. Therefore, these cytokines and chemokines are potential markers for the objective, early detection of mechanically-induced skin damage, such as pressure ulcers.