CHARACTERISATION OF AIRBORNE PARTICULATE MATTER AND RELATED MECHANISMS OF TOXICITY: AN EXPERIMENTAL APPROACH.
- TR Number: 428
- Authors: Bérubé1, K., Balharry1, D., Jones1, T., Moreno2, T., Hayden3, P., Sexton1, K., Hicks1, M., Merolla1, L., Timblin4, C., Shukla4, A., Mossman4, B. 1Cardiff University, Cardiff, United Kingdom, 2Institute of Earth Sciences Jaume Almera, Barcelona, Spain, 3MatTek Corporation, Ashland, MA, 4University of Vermont, Burlington, Vermont. Published in Air Pollution and Health. Editor: Maynard, R.L. Imperial College Press, London, United Kingdom, 69-110 (2006).
- Keywords: 5’-bromodeoxyuridine, Activator Protein-1 (AP-1), Air-liquid interface (ALI), Alveolar Type 2 cell, Ambient particles, Apoptosis, Atmospheric metal aerosol, Bioavailable metals, Cytotoxicity, EpiAirway, FAS/FAS ligand (FASL), Field emission scanning electron microscopy (FESEM), High resolution transmission electron microscopy (HR-TEM), Impaction, Proliferation, ROS, Reactive oxygen, Reactive oxygen species, Thoracic airways, Toxicogenomics, Tracheal/bronchial epithelial cells, Transepithelial electrical resistance (TEER), Tumour necrosis factor (TNF)
- Materials Tested: Acellular lavage protein, Alveolar epithelial cells, Ammonium sulphate, Calcium sulphate (gypsum), ChemVol Model 2400 High Volume Cascade Impactor, DEP, Differentiated epithelial tissues, Elemental organic carbon compounds (EOCC), EpiAirway, Intratracheal instillation, Nasopharyngeal region, Nicotine, Phosphate buffered saline (PBS), Polyurethane foam (PUF), Pulmonary epithelial cells, Residual oil fly ash (ROFA), SV40 T antigen-transformed human epithelial cell lines (BEAS-2B), Tracheal/bronchial epithelial cells
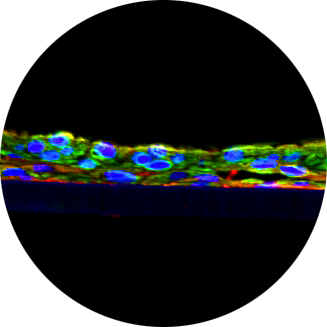
This study by researchers at Cardiff University (UK), the Institute of Earth Sciences Jaume Almera (Spain) and the University of Vermont (USA) demonstrated that MatTek’s EpiAirway human tracheal/bronchial tissue equivalent can be used as an in vitro model to measure the toxicity of nicotine to human respiratory epithelia. For many research laboratories interested in utilizing highly differentiated air-liquid interface (ALI) airway culture systems, it is convenient and economical to obtain fully developed differentiated ALI cultures in a ready-to-use state from commercial sources. One such model system is the EpiAirway™ in vitro human airway epithelial model (MatTek Corp., Ashland, MA). This system is produced from normal human tracheal/bronchial epithelial cells cultured on a variety of individual and high throughput screening culture inserts formats. The cultures display the highly differentiated pseudostratified, mucociliary morphology typical of in vivo tracheal/bronchial epithelium. TEM images reveal additional details of ciliated cells and tightjunctional complexes. Barrier properties of EpiAirway cultures can be evaluated by measurement of transepithelial electrical resistance (TEER). In vivo TEER values are difficult to measure. However, values of about 100-300 Ù x cm2 have been reported for excised tracheal epithelia of various species, including humans (Knowles el al., 1984; Ballad and Taylor, 1994; Joris and Quinton, 1991). EpiAirway cultures typically develop TEER in the range of 300-500 Ù x cm2. The objective of this case study, conducted by researchers at Cardiff University (UK), the Institute of Earth Sciences Jaume Almera (Spain) and the University of Vermont (USA), was to characterise a model of toxicity in human respiratory epithelia, following exposure to nicotine, a particle phase component of tobacco smoke. Nicotine was found to produce a dose-dependent increase in the total protein content of the EpiAirway apical surface wash fluid. There seemed to be a threshold of effect at a 50 mM concentration of nicotine, where the protein content of the wash fluid rose rapidly at higher concentrations. The EpiAirway MTT and TEER assays also showed clear effects with high (125mM) concentrations, producing approximately 50% reduction in MTT and the abolition of epithelial electrical resistance.