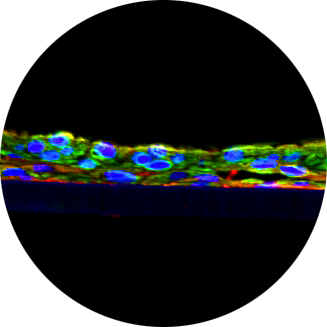
ASTHMATIC AIRWAY EPITHELIUM IS INTRINSICALLY INFLAMMATORY AND MITOTICALLY DYSSYNCHRONOUS.
- TR Number: 581
- Authors: Freishtat1,2,3, R.J., Watson3, A.M., Benton3, A.S., Iqbal1,2,3, S.F., Pillai1,3,4, D.K., Rose1,3, .M.C. and Hoffman1,3, E.P. 1Department of Integrative Systems Biology, George Washington University School of Medicine and Health Sciences; 2Division of Emergency Medicine, Department of Pediatrics, George Washington University School of Medicine and Health Sciences; 3Center for Genetic Medicine Research, Children’s National Medical Center; and 4Division of Pulmonary Medicine, Department of Pediatrics, George Washington University School of Medicine and Health Sciences, Washington, DC.
- Keywords: AIR-606, AIR-606-Asthma, Apoptic cells, Asthma, Bromodeoxyuridine (BrdU), Cell cycle analyses, Dyssynchronous mitosis, Epithelial cells, Epithelial regeneration, Fibrogenic, Flow cytometry, Glucocorticoids, IL-10, IL-13, IL-1β, IL-6, Inflammation, Mechanical injury model, Mitosis, Scrape-wounded, TGF-β1, Wound healing, Wounded area reduction
- Materials Tested: Dexamethasone
Asthma is an inflammatory condition for which anti-inflammatory glucocorticoids are the standard of care. However, similar efficacy has not been shown for agents targeting inflammatory cells and pathways. This suggests a noninflammatory cell contributor (e.g., epithelium) to asthmatic inflammation. Herein, we sought to define the intrinsic and glucocorticoid-affected properties of asthmatic airway epithelium compared with normal epithelium. Human primary differentiated normal and asthmatic airway epithelia were cultured in glucocorticoid-free medium beginning at 248 hours. They were pulsed with dexamethasone (20nM) or vehicle for 2 hours at -26, -2, +22, and +46 hours. Cultures were mechanically scrape wounded at 0 hours and exposed continuously to bromodeoxyuridine (BrdU). Cytokine secretions were analyzed using cytometric bead assays. Wound regeneration/mitosis was analyzed by microscopy and flow cytometry. Quiescent normal (n = 3) and asthmatic (n = 6) epithelia showed similar minimal inflammatory cytokine secretion and mitotic indices. After wounding, asthmatic epithelia secreted more basolateral TGF-β1, IL-10, IL-13, and IL-1β (P < 0.05) and regenerated less efficiently than normal epithelia (+48 h wound area reduction = [mean ± SEM] 50.2 ± 7.5% versus 78.6 ± 7.7%; P = 0.02). Asthmatic epithelia showed 40% fewer BrdU+ cells at +48 hours (0.32 ± 0.05% versus 0.56 ± 0.07% of total cells; P = 0.03), and those cells were more dyssynchronously distributed along the cell cycle (52 ± 10, 25 ± 4, 23 ± 7% for G1/G0, S, and G2/M, respectively) than normal epithelia (71 ± 1, 12 ± 2, and 17 ± 2% for G1/G0, S, and G2/M, respectively). Dexamethasone pulses improved asthmatic epithelial inflammation and regeneration/mitosis. In summary, we show that inflammatory/fibrogenic cytokine secretions are correlated with dyssynchronous mitosis upon injury. Intermittent glucocorticoids simultaneously decreased epithelial cytokine secretions and resynchronized mitosis. These data, generated in an airway model lacking inflammatory cells, support the concept that epithelium contributes to asthmatic inflammation.