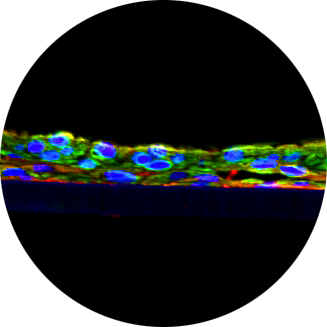
A HUMAN ORAL TISSUE MODEL TO EVALUATE TOXICITY AND ANTI-HIV ACTIVITY OF THE SPERMICIDE-MICROBICIDE, NONOXYNOL-9M.
- TR Number: 429
- Authors: Chang1, M., Klausner2, M., Hladik3, F., Ayehunie2, S., Nittayananta4, W., Coombs1, R.W. 1Department of Laboratory Medicine, University of Washington, 4Department of Oral Biology, University of Washington, 3Program in Infectious Disease, Fred Hutchinson Cancer Research Center, Seattle, WA, 2MatTek Corporation, Ashland, MA.
- Keywords: Buccal tissue, Dendritic cells, EpiOral, EpiOral (ORL-300-FT), EpiOral (ORL-300-FT-LC), HIV, HIV RNA, HIV-1 RNA PCR assay, Human oral epithelial tissue, Human oral full thickness tissue model, Microbicide, Microbicide toxicity, Microbicides, Nonoxynol-9 (N-9)
- Materials Tested: Epithelial tissue , HIV-1 Ba-L, MTT (3-(4, 5-dimethylthiazol-2-yl)-2, 5-diphenyltetrazolium bromide), Nonoxynol-9 (N-9)
This study by researchers at the University of Washington, the Fred Hutchinson Cancer Research Center and MatTek Corp. demonstrated that a new form of MatTek’s EpiOral full thickness human buccal tissue equivalent containing Langerhans Cells appears to be useful in evaluating pre-clinical microbicide toxicity and efficacy. Background: There is a need for a reproducible in vitro tissue model to evaluate pre-clinical microbicide toxicity and efficacy. MatTek Corp., in conjunction with researchers at the University of Washington and the Fred Hutchinson Cancer Research Center, developed a three-dimensional, lamina propria containing, human oral epithelial tissue model and used nonoxynol-9 (N9) as a positive control for the initial evaluation of this model. Methods: Buccal stratified squamous epithelium containing dendritic cells, cultured on a fibroblast-containing collagen matrix and permeable membrane raft (MatTek’s EpiOral ORL-300-FT-LC), was maintained with culture media underneath the basal tissue surface. The integrity of the tissue raft was evaluated daily throughout the study using transepithelial electrical resistance (TER) and viability was assessed at day 3 using conversion of MTT (3-(4,5-dimethylthiazol-2-yl)-2,5-diphenyltetrazolium bromide) by mitochondria dehydrogenase. The apical surface of the tissue was pre-treated with 3.5% N9 (Advantage-S) for 4 hours and washed with phosphate buffered saline (PBS). HIV-1 Ba-L (32 pg of p24 antigen in 40 mcL) was then applied to the apical tissue surface for 8 hours and washed off with PBS. Cell culture media was changed every two days and HIV RNA was measured using a real-time HIV-1 RNA PCR assay. Results: The mean (±SD) epithelial tissue TER at baseline was 229 (±94) ohms (N=54), which increased by 15.8% (±0.28) over 7 days for uninfected tissue (N=5) but remained unchanged [0.34% (±0.21)] following exposure to HIV (N=26). The TER declined by 73.8% (±10.1) from baseline for N9 pre-treated tissue (N=4). Within three days of N9 pre-treatment, tissue viability decreased by 84% compared to controls. Epithelial tissue without dendritic cells did not support infection; however, the incorporation of dendritic cells resulted in HIV infection and the production of sustained levels of HIV RNA for 8 days. Pre-treatment of the tissue with N9 prior to HIV exposure resulted in infection, but with a declining HIV RNA production after 3 days. Conclusions: Our data suggests that HIV-1 Ba-L replicates in the dendritic cell containing three-dimensional model of human buccal epithelium. The integrity and viability of the epithelial tissue model were both decreased by pre-treatment with N9. Limited exposure of tissue to N9 prevented the sustained replication of HIV, which suggests either direct (toxic) or indirect interference with the HIV target cells. The EpiOral tissue model (buccal stratified squamous epithelium containing dendritic cells), ORL-300-FT-LC, warrants further study for evaluating the preclinical toxicity and anti-HIV effect of microbicides.